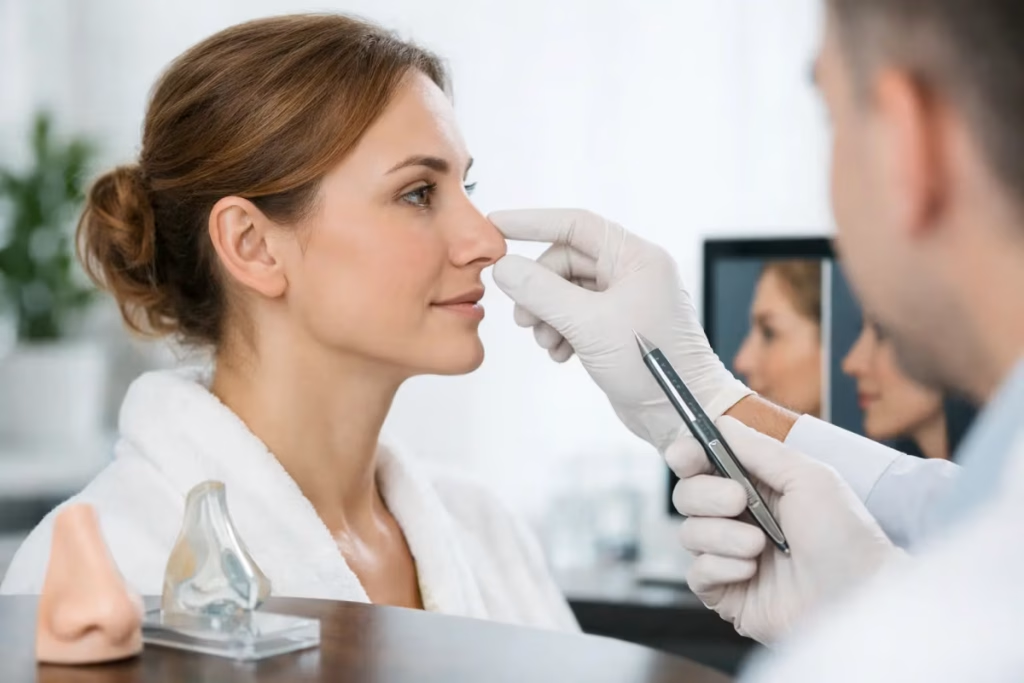
A second nose surgery is rarely just a technical decision. For many patients, it follows disappointment, functional problems, or the feeling that the nose no longer reflects the face with the harmony they originally hoped for. This nose revision guide is written for patients who want a clearer, more sophisticated understanding of what revision surgery can – and cannot – accomplish.
Revision rhinoplasty sits in a different category from primary rhinoplasty. The anatomy has already been altered. Scar tissue may be present. Structural support may be weakened. Skin quality, healing patterns, and breathing dynamics all require closer analysis. In experienced hands, revision surgery can produce remarkable refinement, but it demands more than a standard approach. It requires strategy, restraint, and aesthetic judgment.
Why revision rhinoplasty is more complex
A primary rhinoplasty begins with largely untouched anatomy. Revision surgery does not. Cartilage may have been reduced too aggressively, the bridge may be irregular, the tip may be asymmetrical, or internal valves may have narrowed enough to affect airflow. Sometimes the concern is obvious in photographs. Sometimes it appears only in motion, expression, or breathing.
The challenge is not simply to change what looks wrong. It is to understand why the previous result healed the way it did. A nose that appears pinched may be suffering from structural collapse. A tip that seems heavy may actually be compensating for weak support. A bridge irregularity may become more visible because the overlying skin is thin. This is why revision rhinoplasty is often less about subtraction and more about reconstruction.
In premium rhinoplasty practice, the most successful revisions are guided by both engineering and design. The nose must function as a stable architectural structure, but it must also belong naturally to the eyes, lips, chin, and facial character.
Who is a good candidate in a revision rhinoplasty guide?
The right candidate is not simply someone who dislikes a prior result. Good candidacy depends on the nature of the problem, the condition of the tissues, emotional readiness, and the realism of the goal.
Some patients seek revision because they cannot breathe comfortably after surgery. Others are bothered by visible asymmetry, a drooping tip, excessive narrowing, over-rotation, or an artificial appearance. There are also patients whose first surgery was not necessarily poor, but whose result does not align with their identity. That distinction matters. Revision surgery should address clear concerns, not chase perfection.
A thoughtful consultation explores several questions. Is the problem structural, aesthetic, or both? Has enough healing time passed? Is the skin envelope capable of redraping well? Are grafts likely to be needed? Most importantly, can the patient describe a realistic improvement rather than an idealized transformation?
Timing matters more than most patients expect
One of the most common mistakes after rhinoplasty is evaluating the result too early. Swelling evolves slowly, especially in the tip. Minor asymmetries that look alarming at three months may soften significantly over time. In most cases, revision should not be considered until at least 12 months after the original procedure, and in thick-skinned noses or more complex cases, even longer.
There are exceptions. Severe breathing compromise, infection, trauma, or dramatic structural collapse may justify earlier intervention. But when the issue is mostly aesthetic, patience is not passive – it is part of good surgical judgment.
The reason is simple. Operating on a nose that is still healing makes assessment less reliable and tissue handling more difficult. A surgeon needs to see the stable result, not a temporary phase of swelling and scar maturation.
What surgeons evaluate before revision surgery
A serious revision rhinoplasty guide should go beyond surface concerns. Consultation should include external examination, internal nasal analysis, review of prior surgery details if available, and a frank discussion of limitations.
Skin thickness is critical. Thin skin reveals even slight contour irregularities. Thick skin can hide definition and resist delicate refinement. Scar tissue can distort the normal planes of surgery and make every maneuver less predictable.
Cartilage support is another major issue. If too much septal cartilage was used in the first operation, additional grafting may be needed from the ear or rib. This does not automatically mean a dramatic surgery, but it does mean the revision plan must account for both aesthetics and structural reinforcement.
Facial proportions also deserve attention. Patients often focus on one visible flaw, but revision decisions should be made in relation to the whole face. The elegant result is not the smallest nose. It is the most balanced one.
Common reasons patients seek revision
The motivations are often more layered than they first appear. A patient may say the tip looks “off,” but the underlying issue could be asymmetrical cartilage support, scar contracture, or over-resection from the first surgery. Others report that the nose looks fine in some angles but harsh in others, which may point to subtle contour issues or imbalance between the bridge and tip.
Frequent concerns include persistent deviation, pinched nostrils, collapsed valves, dorsal irregularities, an overly scooped profile, inadequate projection, over-projection, residual hump, and a nose that looks surgically altered rather than naturally refined. Breathing complaints are especially significant because they suggest a functional deficit that should never be dismissed as secondary.
In higher-level revision work, the goal is not only correction. It is restoration of credibility to the nose – a result that appears convincing, stable, and in harmony with the patient rather than visibly “done.”
Surgical strategy in revision rhinoplasty
Revision surgery is highly individualized, but the principle is consistent: preserve what still works, rebuild what has been weakened, and refine only where refinement is truly sustainable.
That often means grafting. Cartilage grafts can restore support, smooth contour transitions, widen compromised internal valves, or improve tip shape. In revision surgery, grafting is not a sign that something has gone wrong in the new plan. It is often the foundation of a durable plan.
Open technique is frequently preferred because it allows broader visibility and greater control in scarred anatomy, though not every revision requires the same level of exposure. The exact method depends on the degree of distortion, the need for structural work, and the quality of remaining tissue.
What patients should understand is that revision rhinoplasty is not always about making the nose smaller. In many secondary cases, making the nose stronger is what ultimately makes it look better.
The trade-offs patients should hear clearly
An honest revision rhinoplasty guide must include trade-offs. Revision surgery can improve asymmetry, breathing, contour, and proportion, but it is typically less predictable than a first operation. Healing may be slower. Swelling can last longer. Scar tissue can influence the final result in ways no surgeon can fully control.
There is also a philosophical trade-off. Some patients want every small imperfection corrected. But aggressive revision in pursuit of microscopic symmetry can increase risk and reduce softness. The most sophisticated outcomes often come from selective correction rather than overworked perfectionism.
This is where surgeon judgment becomes decisive. Technical skill matters, but so does knowing when to stop. The best revision result is usually the one that looks composed and believable, not excessively manipulated.
Choosing the right surgeon for a second operation
Revision surgery is not the setting for bargain decision-making or volume-based marketing. Patients should look for a surgeon with deep rhinoplasty focus, clear experience in secondary cases, strong command of nasal function, and an aesthetic philosophy that favors natural facial integration.
Before-and-after results should be evaluated carefully. Look beyond dramatic changes. Study whether the noses suit the individual faces, whether the tip work looks stable, and whether the profile remains elegant without appearing overdone. It is also worth asking how the surgeon plans complex cases, whether grafting is used comfortably, and how breathing is protected.
At a specialist practice such as DRGO Clinic, revision planning is approached as both structural reconstruction and facial design, which is exactly the level of nuance this category demands.
Recovery and the emotional side of revision
Patients often enter revision with more anxiety than they had before their first surgery. That is understandable. They are not just recovering from an operation. They are recovering from a previous experience that may have shaken trust.
Postoperative swelling can trigger old fears, especially in the early months when the nose does not yet look settled. This is why expectation management is not a soft extra. It is part of quality care. Patients need a realistic timeline, a clear explanation of what will improve gradually, and confidence that slow refinement is normal.
The emotional goal of revision is not only to change the nose. It is to restore ease – in the mirror, in photographs, in social life, and in breathing. That kind of result is never accidental. It comes from patient selection, careful analysis, and a surgeon who understands that a secondary nose must be rebuilt with precision and restraint.
If you are considering revision, look for a plan that respects both structure and identity. The best second surgery does not erase your face. It brings it back into balance.